Fax #: 801-377-3697



Journal of Muscle IQ

Journal of Muscle IQ - Volume 2
September 2023
RESEARCH ARTICLE: Identifying the Reflexive Origin of Muscle Weakness Through Observation of the Myotatic and Autogenic Inhibition Reflexes
Journal of Muscle IQ - Volume 2 - September 2023
Authors: Christopher P. Knudsen, DPT and Alyssa Stewart (PT Tech, BYU Student)
Key words: Muscle Weakness, Muscle Inhibition, Afferent Input, Fascia.
ABSTRACT:
Physical therapists treat muscle weakness in patients every day in outpatient clinics. Most muscle weakness found through manual muscle testing is due to a loss of the Myotatic reflex (or stretch reflex), and/or due to stimulation of the Autogenic Inhibition reflex. This paper will discuss how to identify where the reflexive weakness originates based on testing of the Myotatic reflex. We summarize the science behind the myotatic reflex, the Autogenic Inhibition reflex, and the role of nociceptors in the Fascia in muscle inhibition and the impact of negative Afferent Input messages received by the spinal cord. The reflexive evaluation method will be explained in great detail using real patient cases in the clinic. Videos will be included to better explain the actions involved in this process and the responses from the patients. REFLEXIVE TESTING METHOD: How to Identify the Reflexive Origin of Weakness: Step 1: Perform manual muscle testing to find the weak muscle. Step 2: Test for loss of Myotatic Reflex of a test limb during contraction of the weak muscle. Step 3: Identify the reflexive origin of the muscle weakness. Step 4: Treat the site. Step 5: Retest the Myotatic reflex and retest the weak muscle. CONCLUSION: Most muscle weakness found in the outpatient clinic is reflexive weakness and we can use reflex testing to identify the origin of that weakness. Muscle strength can be restored through treatment at the reflexive origin of that weakness. Physical Therapists with a basic understanding of manual muscle testing and reflexes will be able to replicate this technique with their patients in an outpatient setting and test the premise of this paper, that most muscle weakness found in the outpatient clinic can be linked to reflexive weakening. More case study papers should be written to explain the impact of the loss of myotatic reflex on specific injuries found in the outpatient clinic.




INTRODUCTION:
What is muscle weakness? Muscle weakness is a lack of strength in the muscles. Muscles contract when motor neurons fire in the spinal cord, stimulating the contractile elements of muscle fibers in the muscle. The force of the muscle contraction is dependent on the firing rate of the motor neurons and the number of muscle fibers recruited. Muscle activity is not completely silent during rest, and motor neurons continue to send a baseline level of electrical signals to muscles to maintain muscle tone and readiness. This is known as "resting muscle tone" or "tonic activity."
When the neuromuscular system is in a healthy state, the firing rate of the motor neurons is proportional to the activity being performed. Here are some general motor neuron firing rates for specific activities:
-
Resting: 1 to 10 Hz
-
Walking: 20 to 50 Hz
-
Swimming: 20 to 50 Hz
-
Cycling: 20 to 50 Hz
-
Running: 50 to 100 Hz
-
Jumping: 100 to 200 Hz
When there is an injury, the neuromuscular system is affected, and the firing rates of the motor neurons will be suppressed. This is called Muscle Inhibition.
What is MMT Really Testing?
The use of manual muscle testing (MMT) in outpatient physical therapy clinics is an integral part of the initial evaluation of a patient. MMT scores give us objective measurements that can be submitted to the PCP or insurance company to justify payment for patient treatment. MMT can also be an important tool during every treatment visit to steer treatment to better outcomes when it is thought of as testing the patient’s current muscle reflex health. The authors of this paper feel that MMT is really a test of reflexes. If retesting of the weak muscle after treatment results in a higher MMT then the test is not testing the physical strength of the muscle, but the current state of the body’s reflexes.
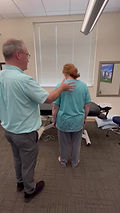
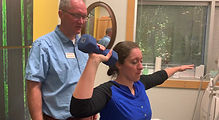
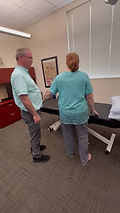
Patient Example: John Doe (32 years old). The patient presents to the clinic with a right ankle sprain. This is their 4th ankle sprain over several years. The patient is sitting on a treatment table with their legs hanging down. (Step 1) MMT of the ankles shows ankle inversion strength on the right to be 3+/5. (Step 2) The patient holds out their right arm to 90’ of abduction and the therapist pushes down on it. The patient can easily resist, and their arm remains abducted. This shows that their myotatic reflex is intact. The patient is asked to turn their right ankle into inversion and hold it there. The therapist pushes on the right arm again and the patient is not able to resist the force (stretch) to their right arm. They have lost the myotatic reflex in this arm. A test of the left shoulder has the same result. It is a global loss of the myotatic reflex due to the patient actively engaging the right ankle into the weak position, triggering the autogenic inhibition reflex, which turns off the myotatic reflex in the rest of the body. (Step 3) While the patient continues to hold their right ankle into inversion, the therapist pushes on the right arm with one hand and palpates the spine from bottom to top with the other hand. The therapist will feel a sudden return of “solidness” to the patient’s abducted shoulder at some spot in the spine. (Step 4) Treatment is then given to that area by the therapist. The therapist can use whatever treatment method they feel is most appropriate for this site. (Step 5) After the treatment is given, the patient is again re-tested as in Step 2, and then again retested as in Step 1. The patient’s MMT of the right ankle inversion is now 5/5.
This patient had a long history of spraining his right ankle because the myotatic reflex kept shutting off in the ankle muscles. Without the aid of the myotatic reflex (or stretch reflex) the muscles will respond too slowly to protect the ankle ligaments from a quick force. The injured tissues in the low back near the spine are what triggered the autogenic inhibition reflex, causing the initial loss of the myotatic reflex in the ankle, prior to the ankle sprain. Once the ankle ligament is sprained, the damaged tissues themselves in the ankle trigger their own autogenic inhibition reflex, making the ankle muscles even slower and weaker. Full long term recovery of this ankle injury will require prolonged treatment to both the injured tissues in the low back and the ankle.
REVIEW OF THE MYOTATIC REFLEX
The NIH states that, “the stretch reflex or myotatic reflex refers to the contraction of a muscle in response to its passive stretching. When a muscle is stretched, the stretch reflex regulates the length of the muscle automatically by increasing its contractility. When a muscle lengthens, the muscle spindle located inside the muscle is stretched, and the rate of neural firing of muscle spindle afferents increases. This augments alpha motor neuron activity in the anterior horn cell pool, causing the muscle fibers to contract and therefore resist the stretching. Another subset of neurons then directs the antagonistic muscles to relax by the mechanism of reciprocal inhibition and in this way the entire reflex process functions to maintain the muscle at a constant length. Gamma motor neurons regulate how sensitive the stretch reflex is by tightening or relaxing the fibers within the spindle.”
Physical therapists stimulate the myotatic reflex every time they manual muscle test. The therapist is attempting to passively stretch a muscle while the muscle is contracted and the muscle responds reflexively to resist this stretch. The same myotatic reflex kicks in during normal functional activities as muscles reflexively contract to resist the forces placed upon them, such as when someone steps off a curb unexpectedly. The brain did not have to make any calculations about how much force the leg muscles needed to generate in order to keep them from falling to the ground. The muscles just reflexively resisted the ground because of the myotatic reflex, keeping the person upright and moving onward. The muscles will reflexively resist and try to match any unexpected applied force.
REVIEW OF THE AUTOGENIC INHIBITION REFLEX
Activation of Golgi tendon organs can result in inhibitory signals being sent to the spinal cord, effectively dampening the myotatic reflex to prevent excessive contraction of the injured muscle. This mechanism is known as autogenic inhibition.
This is the body's way of protecting an injured area and preventing further damage. It's important to note that while these inhibitory mechanisms serve a protective purpose, they also contribute to muscle weakness and altered movement patterns as the body tries to recover from injury.
Inhibitory postsynaptic potentials are signals that essentially put a brake on the motor neurons, preventing them from firing too much and causing excessive muscle contraction. These inhibitory signals come from negative afferent input, which can originate from structures like Golgi tendon organs. These organs sense tension in the muscle and act as safety measures to prevent the muscle from overstretching or contracting too forcefully. When they detect excessive tension, they send inhibitory signals that dampen the activity of the motor neurons controlling the muscle, effectively reducing the muscle's contraction.
Positive Neuromuscular Adaptations: Long-term training and conditioning can lead to neuromuscular adaptations. Athletes, for example, may develop a higher threshold for GTO activation due to their specific training regimens. This allows them to generate more force without triggering GTO inhibition.
Negative Neuromuscular Adaptations: Acute injuries and chronic overuse injuries can also lead to neuromuscular adaptations. Someone in a car accident, for example, may develop a lower threshold for GTO activation due to: Nociceptor activation; thickening of fascia in the injured area; and release of inflammatory chemicals into the system such as prostaglandins, bradykinin, cytokines, and substance P. These all reduce the amount of force the person can generate without triggering GTO inhibition.
What is Afferent Input?
Afferent input, in a technical context, refers to sensory information transmitted from the periphery (such as sensory receptors in the skin, fascia, muscles, and organs) to the central nervous system (the brain and spinal cord). This sensory input is carried by specialized neurons known as afferent neurons or sensory neurons.
Here's a technical description of afferent input:
Afferent input consists of electrochemical signals generated by peripheral sensory receptors, primarily nociceptors, mechanoreceptors, thermoreceptors, and chemoreceptors, in response to various external stimuli or internal conditions. These sensory receptors are specialized to detect specific sensory modalities, such as pain, pressure, temperature, or chemical changes. The afferent input from Nociceptors play a big role in protective reflexes which make our muscles weak.
How do pain receptors cause muscle weakness?
The pathway from the stimulation of a nociceptor to the inhibition of a muscle involves several steps and the communication between different types of neurons within the nervous system. This process is complex and involves both local and central nervous system interactions. Here's a detailed breakdown of the pathway:
1. **Nociceptor Activation**: When tissue damage or potential harm occurs, nociceptors are activated. Nociceptors are specialized sensory neurons equipped with receptors on their surfaces that detect harmful stimuli, such as extreme temperature, pressure, or chemicals released during tissue damage.
2. **Generation of Action Potential**: When a nociceptor's receptors are stimulated by harmful stimuli, they generate electrical signals called action potentials. These action potentials are like a language that the nervous system understands to transmit information.
3. **Transmission to Dorsal Root Ganglion (DRG)**: The action potentials travel along the nerve fibers of the nociceptor towards a cluster of nerve cell bodies known as the dorsal root ganglion (DRG). The DRG is located just outside the spinal cord.
4. **Synaptic Transmission**: Within the DRG, the nociceptor's nerve fibers make connections with other neurons, particularly interneurons. These interneurons act as relays that can amplify or modulate the incoming nociceptive signals.
5. **Transmission to Spinal Cord**: From the DRG, the nociceptive signals are transmitted into the spinal cord through the dorsal horn. The dorsal horn is a specific area of the spinal cord where sensory information is processed.
6. **Synaptic Communication in Spinal Cord**: Within the dorsal horn, the nociceptive signals synapse (communicate) with various neurons, including interneurons and projection neurons. These neurons process and transmit the incoming nociceptive information to higher brain centers for perception.
7. **Projection to Higher Brain Centers**: Some projection neurons carry the nociceptive signals to higher brain centers, particularly the thalamus and the somatosensory cortex. This is where the brain processes and perceives the pain sensation.
8. **Feedback Loop to Inhibit Muscle**: Simultaneously, a branch of the nociceptive signals travels to other areas of the spinal cord, particularly motor neurons that control muscles. These nociceptive signals can activate inhibitory interneurons in the spinal cord.
9. **Reciprocal Inhibition**: The inhibitory interneurons communicate with alpha motor neurons that control the muscle involved. This communication leads to the activation of inhibitory pathways that suppress the activity of the muscle. This phenomenon is known as reciprocal inhibition.
10. **Muscle Relaxation**: As a result of the inhibitory pathways being activated, the motor neurons controlling the muscle are suppressed, causing the muscle to relax. This relaxation prevents excessive contraction in an attempt to protect the injured area from further damage.
Summary of Reflexive Weakness
It is the belief of the authors that injured fascia causes the stimulation of nociceptors in the injured area, which causes direct muscle inhibition to the local muscle and turns off the stretch reflex for that muscle. This injury also causes a lowering of the threshold for the golgi tendon organ in the muscle. Then, when that muscle is engaged, it is more likely to trigger the golgi tendon organ and stimulate the autogenic inhibition reflex globally throughout the body. This is why when testing the test arm (an abducted arm) it suddenly becomes weak when the patient engages the muscles of the injured area (see “Patient Example”above).